Is Assessing strength and patterns of contractions useful?
In many birth settings people often ask ‘how strong are her contractions?’ or ‘is she having effective contractions? While it may be possible to find out how often contractions are coming, and how long they are lasting – I dispute the idea that you can assess how effective or strong they are this way. This post will discuss contractions and whether it is possible to determine their effectiveness.
A quick history lesson
The idea that birth should be efficient has its roots in the 17th century when men used science to re-define birth (Donnison 1988). The body was conceptualised as a machine and birth became a process with stages, measurements, timelines, mechanisms etc. This is still reflected in current textbooks, knowledge and practice.
The legacy of Friedman’s curve
 In the 1950s Friedman created a graph of labour based on his research with 100 women. These women were subjected to rectal examinations every hour during their labour. You can apparently feel the cervix through the rectum although I’ve never tried this myself. The final graph is the basis for modern assessment of labour progress. However there are variations between hospital policies regarding adequate progress. For example a cervix can open 0.5cm an hour in one hospital and be adequate, whereas in another it must open 1cm per hour to be adequate. Now I could do an entire post (and might do in the future) on the ridiculous notion that you can apply a graph to something as complex and unique as a birthing woman. However, I think the evidence speaks for itself. More than half of all women who experience labor in Australia have their labor induced or augmented. Therefore inadequate progress is the norm… or our definition of adequate progress is wrong.
In the 1950s Friedman created a graph of labour based on his research with 100 women. These women were subjected to rectal examinations every hour during their labour. You can apparently feel the cervix through the rectum although I’ve never tried this myself. The final graph is the basis for modern assessment of labour progress. However there are variations between hospital policies regarding adequate progress. For example a cervix can open 0.5cm an hour in one hospital and be adequate, whereas in another it must open 1cm per hour to be adequate. Now I could do an entire post (and might do in the future) on the ridiculous notion that you can apply a graph to something as complex and unique as a birthing woman. However, I think the evidence speaks for itself. More than half of all women who experience labor in Australia have their labor induced or augmented. Therefore inadequate progress is the norm… or our definition of adequate progress is wrong.
How a contraction works (overview)
Physical component:
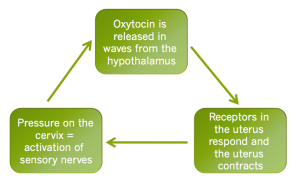 The hormone oxytocin regulates contractions and it is released from the hypothalamus (primitive brain). The uterus has oxytocin receptors which respond to oxytocin by initiating a contraction. Contractions start in the top of the uterus and ‘wave’ downwards. The cervix must be ready (ie. ripe) before it will respond to contractions by opening. This is why induction usually involves preparation of the cervix with prostaglandins before starting a syntocinon (pitocin) drip to create contractions. When the uterus contracts the placental circulation is reduced (more so if the waters have broken), slightly decreasing the oxygen supply to the baby. This is why there are breaks in between contractions – to allow babies to rebalance their oxygen levels before the next contraction. If you’re wanting a reference for the above, any midwifery A&P text book will cover this basic physiology eg. Coad 2005, Stables & Rankin 2010.
The hormone oxytocin regulates contractions and it is released from the hypothalamus (primitive brain). The uterus has oxytocin receptors which respond to oxytocin by initiating a contraction. Contractions start in the top of the uterus and ‘wave’ downwards. The cervix must be ready (ie. ripe) before it will respond to contractions by opening. This is why induction usually involves preparation of the cervix with prostaglandins before starting a syntocinon (pitocin) drip to create contractions. When the uterus contracts the placental circulation is reduced (more so if the waters have broken), slightly decreasing the oxygen supply to the baby. This is why there are breaks in between contractions – to allow babies to rebalance their oxygen levels before the next contraction. If you’re wanting a reference for the above, any midwifery A&P text book will cover this basic physiology eg. Coad 2005, Stables & Rankin 2010.
Note: Oxytocin (syntocinon/pitocin) administered via a drip is not released in waves and an individual woman’s oxytocin receptor response is unpredictable. This may result in contractions that are too powerful without an adequate gap between them leading to a hypoxic baby – similar to what happens during directed pushing.
The psychological / emotional component:
Oxytocin is influenced by, and influences feelings and behavior. There is a growing body of research exploring this aspect of oxytocin and it’s potential uses from treating autism to persuading us to buy products in shops. For real oxytocin nerds like myself,Moberg has written an entire book on how this hormone works. Michel Odent andSarah Buckley are gurus when it comes to the function of oxytocin in birth, mothering and breastfeeding and I would recommend anything written by them. Basically oxytocin is part of the hormonal cocktail that prepares a mother and baby for bonding and attachment. The hormonal formula is: oxytocin (love) + beta-endorphin (dependency) + prolactin (mothering) = mother-baby-bond.
Note: Oxytocin does not cross the blood brain barrier. Therefore, only oxytocin produced in the brain has these psychological/emotional effects. Syntocinon/pitocin administered via a drip into the blood stream only effects the uterus ie. contractions.
Contraction pattern
Contractions are measured according to how often they occur in a 10 minute period and are recorded as 2:10, 3:10, 4:10 etc. To be considered ‘effective’ contractions need to occur 3:10 or more and last for 45 seconds or more. From a mechanistic perspective it would be impossible to progress through labor with 2 contractions or less every 10 mins. .
What I know is that a woman’s contraction pattern is unique. I have witnessed women birth babies perfectly well with very ‘ineffective’ contraction patterns. The recent ones that stand out in my mind are: A woman with an OP baby whose contractions never got closer than 5 minutes apart and were mostly 7-10 minutes apart. And a first time mother who birth her baby with mostly 10 minute spaces between contractions. When left to birth physiologically women’s labor patterns are as unique as they are. Unfortunately many midwives and OB’s are unable to witness a variety of contraction patterns because individuality is not tolerated in the hospital setting.
In my own labors I never have had a consistent pattern. I have been told I have “silent labors” . My last baby after a month of PROM (slow leak another blog) I was forced to induce. Two doses of Cytotec, off and on contractions over 12 hrs. I went from 3 Cm to a baby born in under an hour. Compared to my other 5 labors and births, where I would notice sporadic surges and cramps. Then my midwife would instinctively decide to head my way even though I did not feel I was ready. Only to arrive within 10 minutes of me giving birth. I have given birth to OP babies and LOA babies. My first two were hospital births. With all of my first 5 births my babies came within 10 minutes of my membranes releasing.
Contraction strength
Observing a woman may give you some idea, especially if you have seen a change in her behaviour (sound, movement etc.) over time and/or know her well. But again this is subjective and I’m sure many midwives have been caught out by women who appear to be doing ‘nothing’ but actually are, or appearing to be about to birth when they are not. As the case with myself. I just simply do not feel much of anything except a slight cramping.
Using dilatation of the cervix to determine the effectiveness of contractions is also unhelpful (I have checked myself and have been 2-3 cm at 6 months ). Firstly, routine VEs should not be part of labor care. Secondly, the cervix only shows us one piece of the picture – contractions may have done a fantastic job of rotating a baby and moving him down but not opened the cervix much (eg. with OP position). Thirdly, cervixes open so unpredictably and uniquely that you cannot determine what will occur in the future from what a cervix is doing at a set point in time. A woman can go from a 3cm dilated cervix to birth within minutes or stay at 9cm for hours – cervixes can even close back up.
Sensible assessment of contractions
Induced or augmented labour
 Over-contraction and/or fetal distress are common complications associated with using syntocinon/pitocin in labor. CTG machine may be used to closely monitor the baby’s heart rate. A midwife should also use her hands to assess how often contractions occur, and for how long because CTG machines are not very good at this. Again CTG machines, like midwives/care providers can only tell you how often contractions are occurring and hint at how long they are lasting.
Over-contraction and/or fetal distress are common complications associated with using syntocinon/pitocin in labor. CTG machine may be used to closely monitor the baby’s heart rate. A midwife should also use her hands to assess how often contractions occur, and for how long because CTG machines are not very good at this. Again CTG machines, like midwives/care providers can only tell you how often contractions are occurring and hint at how long they are lasting.
Spontaneous labor
Every woman’s contraction pattern is unique and applying graphs routinely does not improve outcomes and leads to unnecessary intervention. A physically obstructed labor is rare and can be identified by frequent, long lasting contractions over many hours without any change in the position of the baby, or the behavior of the mother, or the cervix. The baby will usually begin to show signs of distress and the mother will ‘know’ that there is something wrong. However, most obstructed labors are psychological/emotional (see above) and if the environment is changed the labor will progress. Indeed observation of the woman and her contraction pattern may actually interfere with her oxytocin release and obstruct her labor.
In summary
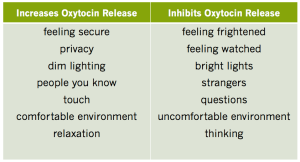
You cannot assess the effectiveness or strength of a contraction. An effective labor pattern is one where mother and baby are well, and there is some kind of progress over time. Instead of assessing contractions, care providers should concentrate on creating an environment that supports oxytocin release. Choosing a home birth is ideal but I realize not all are comfortable with this. Staying home as long as possible to labor is encouraged. If in a hospital setting, not having several in the room or not observing the woman. Avoiding talking to a woman during a contraction is very important for all those attending her birth. As well as a dark room.
~Lisa